Synopsis
Various forms of a thyroidectomy may be advised by your thyroid specialist. In this article, Mr Wale Olarinde (Consultant Thyroid & Parathyroid Surgeon) outlines the different conditions that may require a patient’s thyroid gland (or part of it) to be removed, the consequences/risks of surgery and what to expect.
What is a thyroidectomy?
A thyroidectomy is an operation that involves variations of surgical removal of the thyroid gland
- Total thyroidectomy – whole thyroid gland is removed
- Hemithyroidectomy (thyroid lobectomy) – half of the thyroid gland is removed
- Completion thyroidectomy – half of the thyroid gland is removed, when the other half had previously been removed.
- Thyroid isthmusectomy – when the middle part of the thyroid gland (that joins the right and left sides) is removed.
Thyroid operations may be carried out with other operations such as removal of neck nodes or of the voice box for cancer.
What are the reasons for Thyroid Operations?
Total thyroidectomy – may be advised for a goitre (large thyroid gland that may be causing pressure symptoms on the food tract or wind pipe or may simply be unsightly). A total thyroidectomy is also advised when medication to control an overactive thyroid gland hasn’t worked. Furthermore, a total thyroidectomy may be advised to treat cancer. Thyroid cancer is rare although Mr Olarinde being a thyroid surgeon not uncommonly sees patients with thyroid cancer.
Hemithyroidectomy – usually carried out for a thyroid nodule where it is difficult (after scans and biopsies) to tell if it is cancer or not. A hemithyroidectomy is also carried out to remove a large thyroid cyst.
Completion thyroidectomy – usually carried out after the removal of one half of the thyroid gland has turned out to be cancerous, and it is considered in the patient’s best interests to remove the other half to improve the long-term chance of cure of the cancer. Sometimes a ‘completion thyroidectomy’ may be carried out after one half was removed for pressure symptoms several years ago as the practice was then.
Thyroid isthmusectomy – Done to remove a thyroid cyst or thyroid nodule where it is difficult to tell if it is cancer or not.
What are the options to thyroid surgery
It depends on why thyroid surgery has been suggested in the first place. If it is for an overactive thyroid gland, radio-iodine treatment may be an option if you do not have young children or if your eyes have not been affected by your overactive thyroid gland (i.e. thyrotoxic eye disease). If the reason thyroid surgery has been advised is because of thyroid cancer, there aren’t any options (apart from doing nothing) as surgery is the mainstay of treatment for thyroid cancer. If the reason for thyroid surgery is a large thyroid gland, radio-iodine treatment may be an option although there are limits to how much this will shrink your gland. Radio-iodine treatment may not shrink your gland well enough to relieve the pressure symptoms from your large thyroid gland. A thyroid cyst may be simply left alone or repeatedly aspirated although the latter may not be pleasant.
What to expect with thyroid surgery
Your thyroid surgeon would have investigated your thyroid lump if that is the reason for you needing thyroid surgery. If the reason was an overactive thyroid gland, you are likely to have been referred by your endocrinologist. If you have a goitre, you GP or family doctor would have referred you to a thyroid surgeon who would have requested some preliminary investigations i.e. an ultrasound scan and blood tests.
Occasionally a CT scan may be required if it is felt that there is part of your thyroid gland dipping into your upper chest. A camera examination of your vocal cords (flexible nasoendoscopy) is usually carried out to check that they move adequately before surgery.
Your thyroid surgeon will usually have a detailed discussion about why the operation is recommended and what options you have e.g. simply observing the thyroid nodule, persisting with medication for an overactive thyroid gland or not doing anything about a large goitre if it is not too big or your general health isn’t good enough for you to have surgery. A leaflet about the operation will be issued or sent to you and this forms a nice basis to ask any questions.
You will be admitted on the day of surgery although you would have had an assessment carried out by a nurse to check you are fit for surgery. Some blood tests would have been requested prior to surgery. If you are very healthy (and do not need a general physical examination), your preoperative assessment may have been carried out over the telephone.
What are the inevitable consequences of thyroid surgery?
You will have a scar (depending on how big your thyroid lump or gland is) and this almost always heals very well. There is usually one stitch which is removed anytime from three to seven days after surgery. The scar is hardly noticeable at conversational distance one to three years after surgery. Very rarely scars may be very itchy but this can be helped by emollient cream. There may also be numbness in the first few months around the skin but this gradually settles over time as with any other scar.
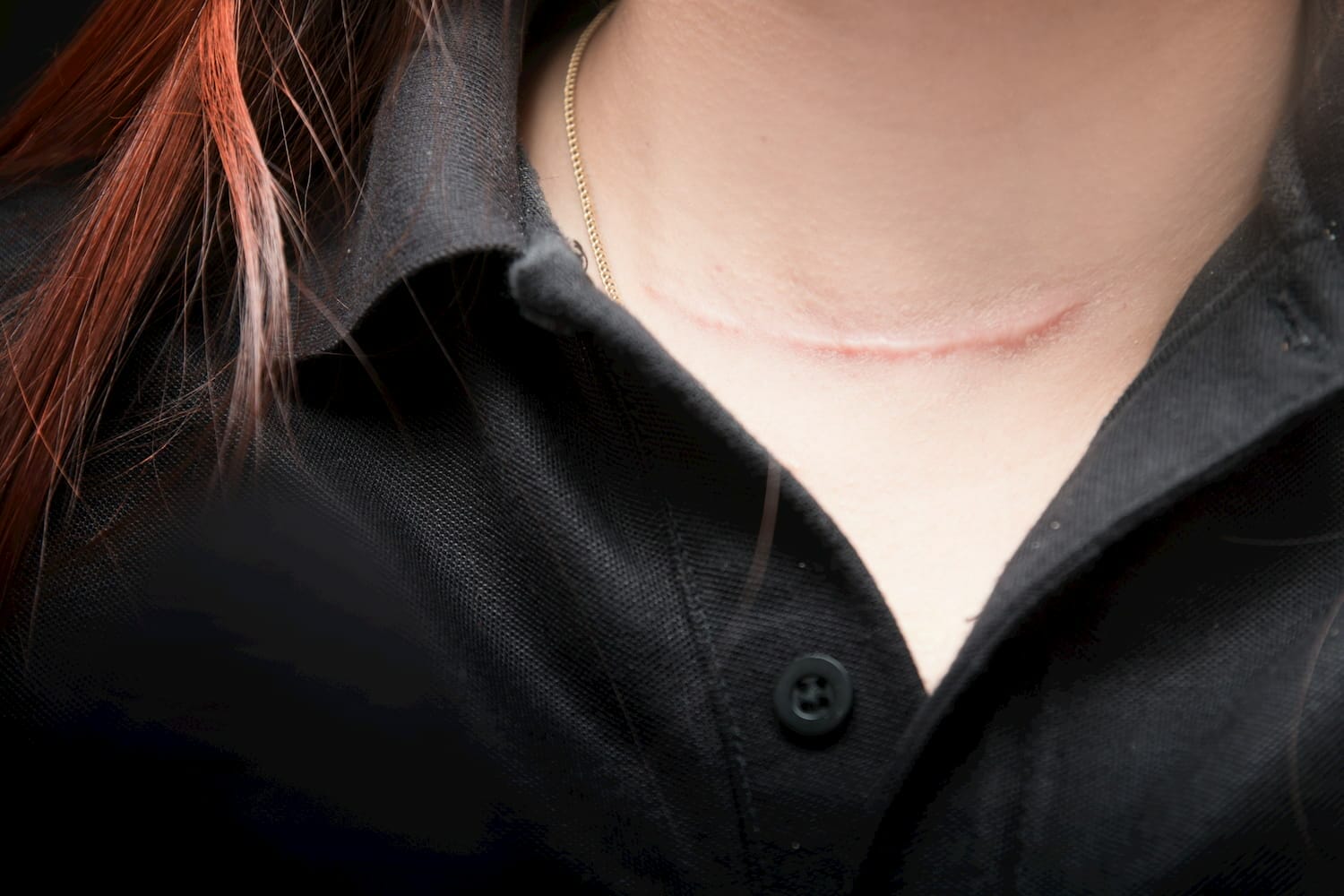
A scar 3 weeks after thyroid surgery
You will be discharged from hospital on the same day after surgery or the day after. Your hospitalisation may however be longer if a drain has been used after surgery. You should be back to normal activity with a week or two after your operation. You can drive as soon as you feel you can move your neck to look over your shoulder. Strenuous activity that may involve neck movements is not advised within the first four weeks. When you return to work depends on what job you do. Most people can return to a desk job within two or three weeks at the most while more physical jobs may mean you being off work for at least four weeks.
If you have had your whole thyroid gland removed, you will need lifelong thyroid replacement. It sometimes takes a few months to get the exact dose your body needs right. The thyroid replacement dose usually increases if you become pregnant.
What are the risks of thyroid surgery?
Thyroid surgery is usually without any complications although things sometimes do not go to plan. The risks of surgery are outlined below
General anaesthetic risks – Thyroid surgery is largely carried out under general anaesthesia i.e. with you completely unconscious. Modern anaesthesia is generally safe and serious problems are very uncommon. Your anaesthetist will usually see you before surgery to discuss any concerns you may have.
Bleeding – may be minimal requiring no active intervention or may be severe enough to require a second operation. Some surgeons use drains although there is no concrete evidence that drains reduce bleeding. Mr Olarinde rarely uses drains except after the removal of very large thyroid glands to keep the dead space (where the large thyroid gland was) collapsed. Mr Olarinde’s risk of bleeding after thyroid surgery is less than 1%. Some patients develop a collection of inflammatory tissue fluid (medical term is seroma). Most of these do not need any active treatment other than watch them recede and get absorbed over time but a seroma may occasionally need to be aspirated or drained.
Hoarseness or voice change – this happens when one of two nerves to the voice box are bruised during a thyroidectomy. Recovery is usually the norm but occasionally complete recovery may not happen leaving you with a hoarse voice or some voice change e.g. inability to shout very loudly. Less than 5% of the patients Mr Olarinde operates on end up with a voice change straight after surgery. Most of those who have any voice change will make a full recovery.
Swallowing difficulties – some patients develop vague swallowing symptoms that almost always settle within a few months after surgery
Calcium levels – if you have had your whole thyroid gland removed i.e. a total thyroidectomy, you may suffer a transient period of low calcium levels where calcium replacement tablets are needed. This is usually because of bruised parathyroid glands. The parathyroid glands are small glands near the thyroid gland that help maintain a good balance between calcium in the blood, gut, bone and kidneys. Occasionally the parathyroid glands may be inadvertently removed. Most of the time the calcium replacement tablets are required for less than three months but there is a slight (less than 10%) risk of needing calcium tablets for life.
Tracheostomy – in very exceptional situations, both nerves that pull the vocal cords apart to enable us breath may be damaged resulting in not being able to breath. This may lead to a tracheostomy where a breathing hole needs to be made in front of the neck to breath. This is a very rare occurrence.
Wound infection – some patients develop a wound infection after surgery. This is rare and the incidence in Mr Olarinde’s thyroid practice is less than 2%. Most wound infections are easily treated with a course of antibiotics used on an outpatient basis. Occasionally a further operation may be required if an abscess develops.
What happens after my thyroidectomy?
Mr Olarinde will usually give you a call or write a letter when he has the report from the laboratory about the nature of your thyroid gland or lump. All specimens are sent to the laboratory to be assessed irrespective of why you needed to have surgery. A follow up appointment usually takes place within about three months after surgery. The camera examination of your voice box is usually repeated to check your vocal cords are moving normally.
